How to stop back or neck pain when reading

How to stop back or neck pain when reading Physiotherapy Column How to stop back or neck pain when reading Written by Caitlin D – Physiotherapist and avid reader. There’s nothing better than getting lost in a good book — until you look up hours later and realise your neck or back is stiff and […]
Why do I have rib pain?

Why do I have rib pain? Physiotherapy Column Why do I have rib pain? Why do I have rib pain? Rib pain is a common form of musculoskeletal pain. It refers to any pain that is experienced in the ribs, the rib joints or the muscles between them. Due to the proximity to the lungs, […]
How to Find the Right Physiotherapist for you!

How to Find the Right Physiotherapist for you Physiotherapy Column How to Find the Right Physiotherapist for you Written by Sal – Director and Founder of Barefoot Physiotherapy in Brisbane. Est 2012 How to find the right physiotherapist for you! I’m going to start this blog by saying we are not for everyone, and that’s […]
Holistic Physiotherapy at Barefoot Physiotherapy: Your Journey to Whole-Body Healing

Holistic Physiotherapy at Barefoot Physiotherapy: Your Journey to Whole-Body Healing Barefoot Lifestyle Column Holistic Physiotherapy At Barefoot Physiotherapy, we are committed to delivering the highest standard of Holistic Physiotherapy to every client. True holistic care means shaping each treatment plan around the unique individual—recognising your goals, lifestyle, and the way your body responds to movement […]
Best Physio Brisbane: Why Clients Choose Barefoot Physiotherapy

Best Physio Brisbane: Why Clients Choose Barefoot Physiotherapy Physiotherapy Column Physiotherapy Brisbane Looking for the best physio in Brisbane? At Barefoot Physiotherapy, we’ve proudly supported the Brisbane community for over a 12 years with expert, holistic care that gets real results. Our mission is simple: to help you feel better, move well, and live life […]
The Thoracic Ring Approach as incorporated in the Barefoot Physiotherapy Plan

The Thoracic Ring Approach as incorporated in the Barefoot Physiotherapy Plan Physiotherapy Column The Thoracic Ring Approach as incorporated in the Barefoot Physiotherapy Plan At Barefoot Physiotherapy we utilise techniques from multiple learnings all combined into our unique Barefoot Physiotherapy Plan. These techniques include; LJ Lee’s training in The Thoracic Ring Approach™all of our Bachelor/Masters […]
Physiotherapy for TMJ
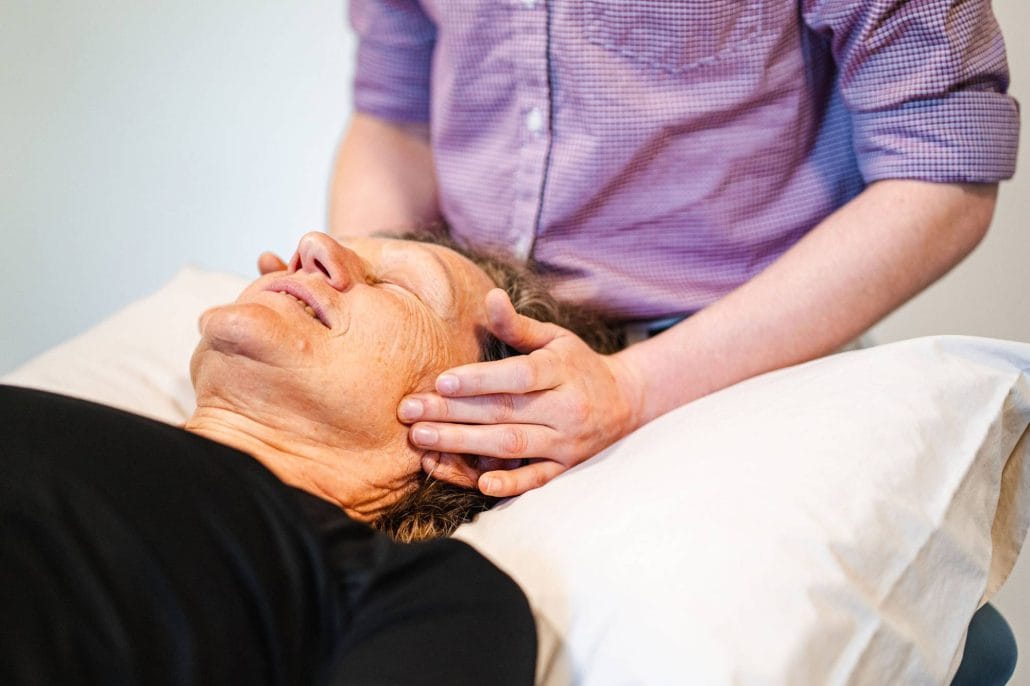
Physiotherapy for TMJ Physiotherapy Column Physiotherapy for TMJ What Is TMJ? Have you ever wondered if something is wrong with your jaw, or asked yourself “why is my jaw clicking?” Perhaps you have been told by your doctor or dentist that you have something called “TMJ dysfunction.” What does this actually mean? And how can […]
How to Relieve Pelvic Girdle Pain During Pregnancy

How to Relieve Pelvic Girdle Pain During Pregnancy Physiotherapy Column How to Relieve Pelvic Girdle Pain During Pregnancy Throughout pregnancy, many women will experience some form of Pelvic Girdle Pain (PGP). Knowing how to relieve pelvic girdle pain during pregnancy is vital to ensure women still have a good pregnancy experience and one that allows […]
Activity pacing

Activity Pacing Physiotherapy Column Activity Pacing Activity pacing is a vital component of physiotherapy management for chronic conditions. It is an approach that involves balancing activities throughout the day to prevent overexertion and conserve energy. This technique is particularly useful for individuals who experience chronic pain or fatigue, as it can help manage symptoms and […]
Women are not Small Men – A Physiotherapy Perspective

Women are not Small Men – a physio perspective clinicians corner Women Are Not Small Men: Why Understanding that Matters in Health and Performance WRITTEN FOR CLINICIANS – From Caitlin Sargent’s training with Stacey Sims. For far too long, the health and performance needs of women have been underrepresented in research and practice. From sports […]
