Energy Debt: Functioning But Not Recovering
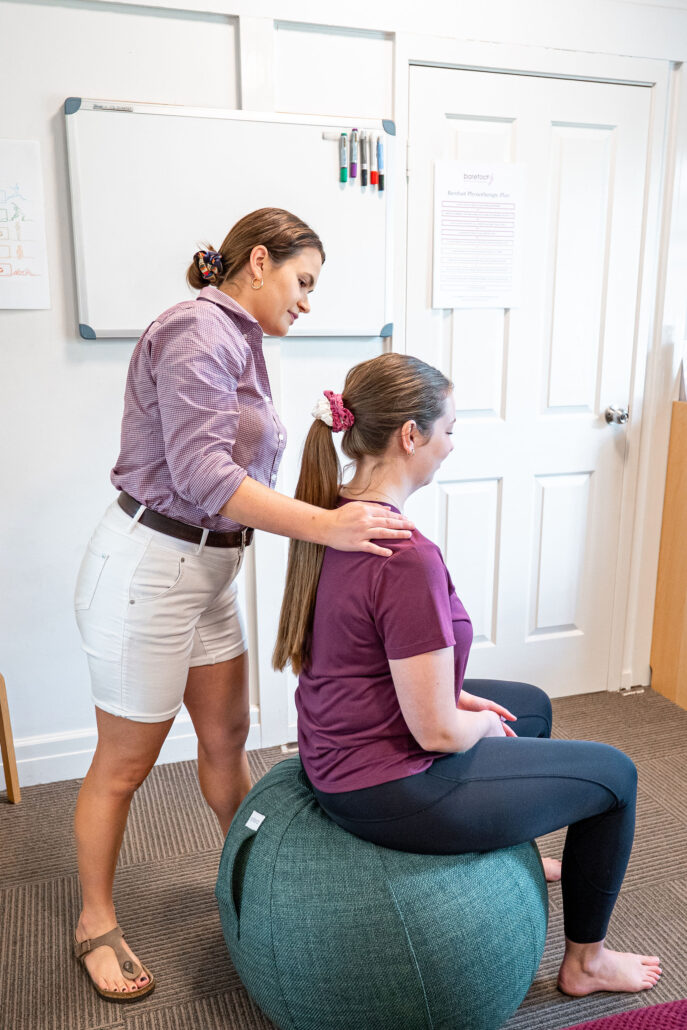
Energy debt: When you are functioning, but not recovering Physiotherapy Column WRITTEN BY: SAL OLIVER LANGE – DIRECTOR/HEAD OF PHYSIOTHERAPY ONE OF THE MOST COMMON PATTERNS WE SEE AT BAREFOOT IS HIGH-FUNCTIONING PEOPLE RUNNING ON A DEFICIT. NOT BROKEN. NOT FAILING. JUST OUT OF BALANCE. THE WORLD IS A LOT RIGHT NOW AND HONESTLY I’M […]
Why Women Need to Put the Oxygen Mask on First

Why women need a reminder to put the oxygen mask on first Physiotherapy Column We’re living in a culture of hustle. People are working more, carrying more, trying to achieve more, and doing it all at speed. Even the ‘healthy’ things can start to look like another task to complete. What we see at Barefoot is a lot of brilliance […]
NSAIDs and Pain Relief: What You Need to Know | Barefoot Physiotherapy

NSAIDs and Pain Relief—What You Need to Know Physiotherapy Column Written by: Sal Oliver Lange – head of Physiotherapy At Barefoot Physiotherapy, we’re here to support your whole health – not just your pain. Part of that includes helping you understand your options, including when medication might play a role in your recovery. One group […]
Holistic Physiotherapy Brisbane | Whole-Body, Individualised Care

A complete guide to whole-body treatment Physiotherapy Column At Barefoot, we believe most people don’t need tougher motivation – they need better clarity. We believe in taking your story seriously, looking beyond the sore spot, and using testing and re-testing to reduce guesswork. And we believe real progress usually comes from the slower moments: the ones where […]
Asking the body what it wants
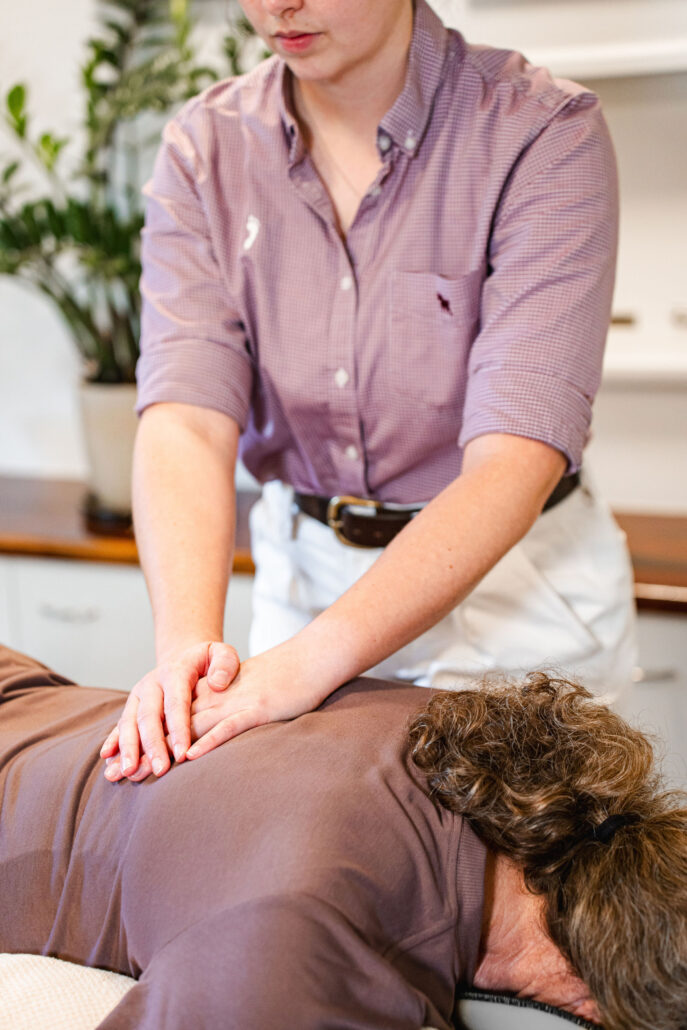
Asking the body what it wants Physiotherapy Column Why R1 and Treatment Direction Tests Change Everything There’s a moment in almost every Barefooters treatment journey where we make a change together and we both get excited – the client and the physio! Usually this is in a Range of Motion test or Neurodynamic nerve test – but it could be in anything […]
Easy Tips for Muscle Releases at Home

Easy tips for doing your muscle releases at home Physiotherapy Column Why being kind to your body actually helps recovery At Barefoot Physiotherapy, we’re big believers in helping people feel more at home in their bodies, not just during appointments, but in everyday life. One of the simplest (and most effective) ways to support your body between […]
Compassion and healing: why being kind to your body actually helps recovery

Compassion & healing Physiotherapy Column Why being kind to your body actually helps recovery At Barefoot Physiotherapy, we see it every day: healing works best when the body feels safe, supported, and understood. Movement, strength and rehab matter, but so does how we treat ourselves during recovery. One of the most overlooked tools in healing is compassion. Not the […]
Brain Overload: When Your Body Tells You to Stop

Brain Overload Physiotherapy Column Brain Overload: When Your Body Tells You to Stop We all have a lot going on: work, family, friends, deadlines, goals, and the never-ending to-do list. So when your body starts showing signs of pain or stiffness on top of all that? It can feel like the last straw. But here’s […]
Inclusive LGBTQIA + Physio in Brisbane

Inclusive LGBTQIA + Physio in Brisbane Physiotherapy Column Inclusive LGBTQIA + Physio in Brisbane – WRITTEN BY: SAL (SHE/HER) – FOUNDER OF BAREFOOT PHYSIOTHERAPY. Truly inclusive healthcare is a fundamental human right and underpins every part of the Barefoot approach. The philosophy behind the clinic is simple: empower people to confidently live the lives they […]
Why Back Pain Keeps Coming Back (And What Helps)

Why back pain keeps coming back (and what helps) Physiotherapy Column If your back pain keeps coming back, you’re not imagining it. You might have a few better days. Maybe even a good week. Then something small happens. You sit a little longer than usual. Sleep badly. Lift something light. Have a stressful week. And the pain is back […]
