Self-Releases vs Stretching: When, Why and the Benefits
in Case Study Treatment, Physiotherapy ColumnIf you have been to a Physiotherapist before, there is a good chance you have been prescribed a muscle self-release (Usually performed with a ball) or a muscle stretch of some kind as homework. At Barefoot Physiotherapy, both are prescribed, and for slightly different reasons. Below, we will go through the benefits of Self-Releases vs Stretching and when each are appropriate.
 Benefits of both self-releases and stretching:
Benefits of both self-releases and stretching:
- Decrease in tension/discomfort in the muscle
- Potential to lengthen the muscle and increase joint range of motion
- Enhance performance
- Can improve motor control
- Can improve posture
The main prescription differences Self-Releases vs Stretching:
- Nerves have the potential to be irritated with stretching. This is why if a client has any neural irritation, we avoid prescribing stretching until that neural irritation has been cleared. This decreases the chance of aggravating any nerves, and consequently speeds up the client’s recovery.
 General tight muscles vs. “knots”. A lot of tight muscles have palpable “knots or trigger points” in them. These are in certain areas and not throughout the entire muscle. To target these, muscle releases (With a ball, pocket physio or foam roller) are more effective than stretching the entire muscles. The mechanism of benefit is similar to that of a therapeutic massage, and relies on pressure to the muscle to relieve tension and increase efficiency of the muscle fibres.
General tight muscles vs. “knots”. A lot of tight muscles have palpable “knots or trigger points” in them. These are in certain areas and not throughout the entire muscle. To target these, muscle releases (With a ball, pocket physio or foam roller) are more effective than stretching the entire muscles. The mechanism of benefit is similar to that of a therapeutic massage, and relies on pressure to the muscle to relieve tension and increase efficiency of the muscle fibres.- Stretching on the other hand can be a more effective prescription if the client has an entire muscle group that is notably tight.
- Studies have shown athletic performance benefits when dynamic stretching is used prior to competition.Although there are minimal (if any) studies examining muscle releases immediately prior to athletic performance, we propose that daily muscle releases are also beneficial to performance.
- Performing regular muscle releases can decrease muscle tension and “knots”, and therefore likely benefit athletic performance, similar to stretching.
It is important to understand the benefits and risks of muscle Self-Releases vs Stretching so they can be used safely and effectively. If you have any questions about Self-Releases vs Stretching with your specific exercise program or training regime, ask you physiotherapist or contact us at Barefoot Physiotherapy 🙂
Our friends at Amber Tree Yoga also have a regular release class worth checking out.
Returning to Sport after Injury
in Case Study Treatment, Physiotherapy ColumnHere at Barefoot, a lot of our clients present to us with an injury they sustained during sport. From dance to yoga and football to power-lifting, there is nothing more frustrating than having an injury prevent you from doing the activity you love. The most common question in returning to sport after injury, is how long should I wait? or get treatment for?
Other questions such as:
- How long until I can get back to running?
- How long until I can compete again/re-join my team?
- If I play will I re-injure myself again?
There are some injuries with healing time-frames which dictate roughly the minimum amount of time an athlete will spend in recovery. For example a bone fracture or a complete rupture of a muscle or ligament will have very specific time-frames (and possibly surgical involvement) which will prevent someone from returning to sport within those first couple weeks…
Over the next few paragraphs we’ll discuss sporting injuries, and the approach we take to them at Barefoot Physiotherapy, and how we determine if an athlete is ready to return to their sport.
The most frequent types of injuries we see in clinic are ligament, muscular and tendon soft tissue injuries – of varying degrees.
The steps we take at Barefoot when aiming to get someone returning to sport after injury (After acute management has been given):
- First and foremost – we need the athlete to have no nerve irritation. An athlete with nerve [neural] irritation stemming from the spine will not recover as fast as one who is neural clear. When nerves are irritated (as shown objectively on our Neural Dynamic Tests) the muscles around them tense up and may spasm to protect the nerve. This reduces movement and places higher forces on joints/structures in the body, consequently taking the body longer to recover. If not cleared fully it also predisposes them to further injury. This is a crucial step.
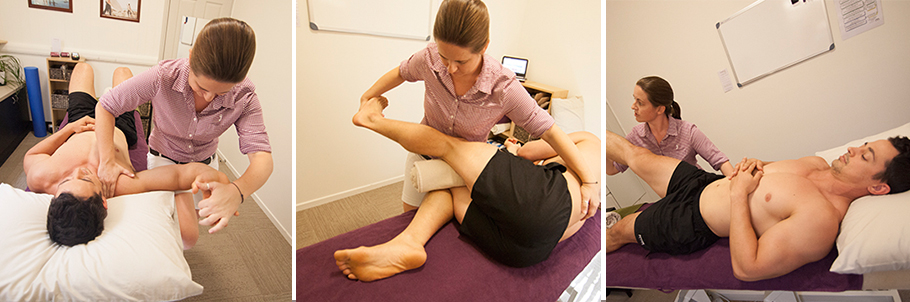
- Appropriate Ranges of Motion (Ideally throughout the entire body – and definitely equal on both sides of the body). By going through the Barefoot Plan, we will determine areas of the body contributing to reduced ranges of motion, and treat those accordingly until an athlete has full range.
- Full Strength and Proprioception about the affected joints – To regain strength and balance, steps 1 and 2 need to have been addressed. The actual strength gains itself will be developed through a therapeutic, sport specific graded exercise program prescribed by one of Barefoot’s Physios or one of the trainers who we commonly refer to.
- By this point in an athletes rehabilitation, pain should be substantially diminishing, if not completely gone.
- Once steps 1-3 have been accomplished, it is now time to think about actually getting this athlete returning to sport. This is done by starting with the most basic principles of their chosen activity, and working our way up to the most complex/challenging aspects of it. To truly be able to determine if someone is ready for returning to sport at 100% intensity, we recreate their sport specific environment, and assess their performance.
- If the client has any pain, discomfort, imbalance or poor motor patterns during the assessment of their abilities…then they are surely not ready to SAFELY return to sport at this time. See below example for returning to sport for a soccer player
For example, assessing a soccer player’s ability to return to sport would involve:
- Running in a straight line – slow pace, no change in speed no change in direction
- Then in a straight line – medium pace, no change in speed no change in direction
- Followed by running in a straight line – fast pace, no change in speed no change in direction
- Then Zig-zag between pylons – slow pace, no change in speed
- Repeat at moderate to fast speeds
- Finally running backwards, then turning and running in the same direction forwards – slow pace
- Repeat at moderate and full speeds
- Soccer ball skills
- Passing a soccer ball short distance (1m) – inside of the foot
- Repeat at moderate and long distances
- All of step 6 above with a top of the foot pass
- Again all of step 6 with right and left foot
- Dribbling the soccer ball
- Slow pace
- Moderate pace
- Fast pace
- All of the above performed in a straight line, and in varying pylon set ups (zig zags)
- Incorporate an unstable environment:
- Steps 1-5 re-performed without the athlete knowing which way they are going to run
- Example: Athlete running at a moderate pace towards Physio, at the last second Physio will point either right or left and the player has to sprint for 3 seconds in that direction
- Steps 1-5 re-performed without the athlete knowing which way they are going to run
- Combination of steps 1-5 with steps 6 and 7
- Incorporating running with ball control
- Example: get the athlete jogging, not knowing when the Physio will pass her the ball, and when it’s passed, having her pass it back immediately with one touch.
- This can be incredibly variable, and will start slow and steady and progress to full speed drills in an unstable environment, where the athlete has to change their speed, change their direction and perform sport specific (soccer ball) skills, all on one drill.
The Assessment
The assessment above is done in such an order (most basic drills to the most challenging) because we want to know immediately if there are any concerns with the athletes’ injury recovery. Unless all of the above can be performed with no concerns, then we would not be happy to tell somebody that they are ready to be returning to sport.
The above example is a fairly basic one. At Barefoot Physiotherapy, returning to sport assessments are tailored to the individual and their specific position and or role in their chosen activity.
Our Job at Barefoot
Athlete safety and recovery is of the utmost importance, and we are here to support you. As part of your support system, it is our job to take you through the above steps, and make sure you are FULLY RECOVERED before we give you our OKAY to return to your chosen activity. There is nothing worse than being told you are recovered, and going out and re-injuring yourself.
If you have any sport specific questions about rehabilitation, please do not hesitate to ask 🙂
Happy sporting!
Fat Ankles from Flying
in Barefoot Lifestyle, Case Study TreatmentDo you suffer Fat Ankles from Flying? With both domestic and international flights back on the cards, more and more of us are flying. Sometimes these trips can be longer than 2 hours, reaching 13 hours for a long-haul flight, which also might be followed by even more flying. Prolonged sitting, lack of movement, dehydration, pressure on the hips and hamstrings can all contribute to fat ankles from flying.
Sometimes no matter how much you try and move around, swollen ankles can still result.
So, why do we get fat ankles from flying, especially on those long trips? Is this dangerous? How do we prevent it?
Let’s start with why this happens. Whenever we are sitting for a long period of time in a plane, the muscles in our legs that are usually responsible for pumping blood and fluid back up are legs are not being used at all. Over time, this will lead to an increase in fluid and blood pooling in our lower limbs (ankles).
Additionally, on long flights in a low air pressure aircraft cabin, it is easy to forget to drink water. Firstly, the stress of flights sometimes makes an alcoholic beverage a more appealing choice, and secondly a lot of people avoid too much water because they do not want to be getting up and going to the toilets on a regular basis while flying. This makes it very easy to become mildly dehydrated on airplanes. Being dehydrated can reduce your blood circulation, making it that much easier for fluid to pool in your ankles on those long flights.
Is this dangerous? The ankle swelling itself is not dangerous, however the reasons which cause it can also cause things like blood clots or deep vein thrombosis (blood clot in your calf), which can be seriously dangerous and has the potential to cause death. So although the ankle swelling itself is not a reason for concern, the reasons which caused the ankle swelling is definitely reason enough to take it seriously and take any necessary precautions to prevent it.

How do we prevent it?
- The biggest thing you can do to prevent poor circulation and subsequent ankle swelling is movement. Aim to get up on a half hourly basis (Assuming you are not asleep) for a walk around the cabin. Aim to be up walking for at least 3-5 minutes each time.
- It is crucial to stay hydrated. This means drinking water before and during the flights. Even if you are having a glass of wine or a beer, try and also have a bottle of water on the go as well.
- It is important to keep your feet and legs moving as much as possible even while you are seated. Pump your ankles from side to side and up and down on a regular basis.
- Some people wear compression stockings while flying to prevent blood clots in their legs. There is evidence suggesting that wearing these stockings can significantly reduce your chance of a blood clot which is great, however it is important to remember that stockings are NOT a substitute for any other of the above precautionary measures, most importantly exercise and frequent movement on a plane.
- There is research that suggests taking aspirin during your flight slightly thins the blood, reducing the chance of deep vein thrombosis and swelling. However, we strongly recommend checking with your doctor before flying if this is right for you.
- Holding or placing your feet above your heart is obviously a great way to keep the blood from pooling in your feet and ankles. If you can, see if you can lift your knees and legs up high, placing them on the seat in front of you – obviously trying not to annoy the passenger in front of you. Handstands in the space outside the toilets or galley is also a fun way to get the blood moving – don’t knock over the food cart!
- After your flight, when you finally get to lie down, put your legs up the wall. This is awesome to drain the legs lymphatic system, encourage oxygenated blood to circulate up the legs and feet.
- Post-flight massage is also a great way to alleviate any swelling. You could do this yourself, or find somewhere close by that you can walk to. The gentle practice of just walking will also assist the body in circulating the blood.
Of course if the swelling doesn’t go down and/or you’re feeling any discomfort or pain, visit a health care practitioner as soon as you can. We’re also here to help, either with some specific treatment before or after you fly. All of our Physios are very well versed in the affects of flying, and are ready to help you make you feel amazing any time you need. Click Here to book online now.
Falls Prevention and how Physiotherapy can help
in Case Study Treatment, Physiotherapy ColumnAnyone can, and does fall at some point throughout their lives, for most of us it is multiple times. Unfortunately, the older you get the more impact these falls can have. As we get older we need to take further precautions in order to stay safe. We can do this by putting in place some falls prevention techniques.

Here are some falls prevention quick tips for either at home or in the community.
- Stay active and participate in group activities such as Tai Chi, Yoga or Walking.
- Making sure you have good fitting shoes with good gripping soles, and avoid wearing loose fitting shoes (slippers) or socks, especially when walking on a slippery surface.
- Make sure there is enough light for you to see well, especially when walking at night. This does include turning on the lights when getting up in the middle of the night to go to the bathroom.
- Using a walking aid, such as walking stick or frame, when you need to.
- At your house, you can consider putting grip tape on the edge of your stairs.
Physiotherapy’s role in falls prevention can be somewhat underestimated, so how do we help?
Well firstly we are able to fully assess not only your body, but your balance to help determine the level of risk you have to fall. Then once we have determined this, we are able to come up with individualised programs to help decrease this risk. These programs are things that will work on your muscle strength (not necessarily lifting heavy weights), and your balance. For example, standing on one leg in a yoga pose can go a long way to correcting and ensuring good balance.

Falls Prevention
Along with coming up with this program, we are also experts in the adjustment and maintenance or your walking sticks or frames, making sure they are as safe for you as possible. This may mean that we either adjust a frame or stick that you already have, or we may suggest to you that you get one, in order to help prevent any future falls.
We hope you’ve found these tips, tricks for Falls Prevention helpful. We’d love to hear from you if you have further ideas on how to prevent a fall.
If you feel you would love some help from us, you can give us a call, or book on-line for an appointment today!
Physiotherapy for Pain Management
in Case Study Treatment, Physiotherapy ColumnHere’s a great article from our Industry Body explaining the current situation with Codeine becoming prescription only, and how Physiotherapy for Pain Management can be an effective treatment option.
With codeine becoming a prescription only drug from February, a large number of Australians will be seeking alternative ways to manage their pain.

National President of the Australian Physiotherapy Association, Phil Calvert said, ‘The good news is that physiotherapy is proven to provide effective pain relief, which treats rather than simply masks the underlying cause of pain.’
‘We appreciate that restricting access to codeine may cause anxiety for people who suffer an injury. So we want them to know that physiotherapists help people to manage their pain and recover movement with great success, without the use of addictive drugs.’
Research has shown that the relative level of pain that is experienced by someone can be influenced by a range of factors including their emotions and social environment. This means that pain can be a very complex issue to successfully treat.
‘There is no one size fits all approach in assessing and treating someone’s pain. So physiotherapists are practiced in considering a range of factors that may be contributing to the pain. We’ll talk with patients about their lifestyle goals and introduce an appropriate treatment including exercise programs, joint manipulation and mobilisation,’ said Mr Calvert.
What to expect from a physiotherapy consultation:
- Your physiotherapist will perform a physical examination and find out more about your history and any other factors that may be contributing to the pain.
- In most cases of acute pain (the period in which an injury is expected to heal), the pain will settle as the tissue heals. Your physiotherapist will explain the nature of the injury and normal healing times. They may provide early treatment, but in many cases advice regarding self-management strategies, including gentle exercise, will be enough to help resolve the pain and return you to full function.
- In situations where the pain has become chronic (generally more than three months – longer than normal healing times), assessment and management may be more complex. Things other than tissue damage may be contributing to your pain, which your physiotherapist will investigate. In complex situations other specialists may also form part of a wider treatment team.
- At all stages of pain management, physiotherapists will work with you to encourage self-management, remaining active as appropriate and avoiding a reliance on medication.
If you’re experience pain or difficulty with movement that may cause pain, please don’t hesitate to get in touch with us. Here’s a BLOG of ours to read, If you’d like some simple exercises to assist with pain management: https://www.barefootphysiotherapy.com.au/easy-exercises-keep-healthy-active-age/
Functional training, here’s what you need to know!
in Case Study TreatmentHere at Barefoot we’re often asked about buzzwords in the fitness space and a phrase that regularly comes up is functional training. You’ve probably seen the term used in fitness advertising and many trainers offer it as a part of their exercise programming. So we want to discus the functional approach to exercise, the benefit it provides, and give you a few tips on how to ensure your exercise involves a functional component.
Let’s begin with the term functional.

adjective
- having a special activity, purpose, or task.
“a functional role”
- designed to be practical and useful, rather than attractive.
“a small, functional bathroom”
With this definition in mind, the concept of functional training involves performing exercise that has purpose and will be useful to the exerciser. To assess the practicality of the exercise you are currently doing it is worth considering the kinds of movements that are purposeful to you. Or to put it another way, what movements are you required to do everyday in your environment? This varies from person to person and depends on variables such as work, sport, life stage, and personal goals and hobbies. Programming exercise with a functional approach, therefore, must take into account such variables in order to be practical and useful. As it turns out, a majority of the time, the complexity of human movement can be broken down into just a few basic fundamental movements – pulling, pushing, squatting, lifting, and walking/running. When you see “functional training” offered as a part of a fitness service generally speaking it is offering an exercise program that involves training these fundamental human movements. It should also be considering your individual goals and lifestyle.


In many cases exercises that could be considered as “functional” involve movement of multiple joints, action of multiple muscles and ultimately has a basis in fundamental human movement. The reason for this is that this reflects many of the movements of day to day life – think carrying groceries in from the car, picking up and holding children, placing objects up on an overhead shelf, even running to catch a train – each example involves movements of multiple joints and muscles, and has a basis in one of the fundamental human movements – sound familiar?
By performing exercise with a functional approach not only do you receive the benefits of exercise and gain strength but the movements and moments of day-to-day life become easier. If you can train what it is going to be useful to you in the real world environment your ability to carry out physical tasks improves.
This also means your resilience to injury improves too!
Want to make your training more functional? Here are some things to consider.
- Ensure your trainer understands the sort of physical activities you do regularly. This will give them an idea of your movement profile and whether you need to train for strength, power, or endurance.
- If you’re already doing certain exercises ask yourself how the exercise will be useful to you. If you’re told an exercise is functional consider asking “functional for what?”. Often times, exercises involving multiple joints and muscles will be more practical since they mimic the movements of day to day life.
- Keep in mind that not everything we do in our day to day lives needs to be trained in the gym. For example, the best way to train your good sitting posture and build endurance in your postural muscles, is to use your time in the office to practice!
Regardless of the term you use to describe your exercise just remember to move often in a variety of ways and above all find something that you enjoy. Exercise can come in many forms. There’s lifting weights, rock climbing, martial arts, yoga, running, gardening, barefoot bowls…the list goes on. Just be sure to move often and if you find this difficult find something you enjoy as this will make your movement habits easier and set yourself up for success.
Want to know more? Or meet with one of the physios to discuss how you can get your body moving again? Click here.
Knee ligaments and injury
in Case Study TreatmentThe knee is vital for everyday functions, yet it is often poorly understood. There are many misconceptions about what is ‘good’ or ‘bad’ for knees and exactly what is going on inside the joint.
The knee is identified as a hinge joint, meaning it primarily moves in one direction (ie bending and straightening). It is made up of the femur (thigh bone), tibia (shin bone) and patella (knee cap). These bones are all held in place by a number of ligaments. The ‘joint surfaces’ (parts of the bone that glide on one another) are covered in articular cartilage to absorb shock and reduce friction in the joint. The joint capsule and ligaments serve to provide stability to the knee, whilst allowing it the necessary movement.

The main knee ligaments are summarised below:
- Medial collateral ligament: sits outside the joint capsule and runs between the tibia and femur (inside of the leg) to provide resistance to forces pushing the knee inwards
- Lateral collateral ligament: sits outside the joint capsule and runs between the tibia and femur (outside of the leg) to provide resistance to forces pushing the knee outwards
- Anterior cruciate ligament (ACL): is within the knee joint and runs from the front of the tibia to the back of the femur
- Posterior cruciate ligament (PCL): runs from the front of the femur to the back of the tibia (also within the joint)
- Patellar ligament: sits outside the joint capsule and runs from the patella (kneecap) to the front of the shin
The meniscus is another key structure in the knee joint. It is a fibrocartilaginous disc that sits between the tibia and femur to help absorb shock and improve load-bearing of the knee (twisting and stretching).
Common knee injuries
While we see a lot of pain that is a result of a build-up of accumulated strain, there are also a number of injuries that are caused by sudden trauma. These can include a rugby tackle, poor landing in netball, falling over skiing and even your form during rock climbing.

While accumulative strain injuries are usually the result of tight or weak muscles and stiff joints, traumatic injuries may involve structural damage to the knee joint.
Stay tuned for next weeks blog post, where we will discuss common knee injures, what causes them and most importantly, how to treat them.
If you would like to learn more, or visit one of our physio’s click here!

Acknowledgement of Country
Barefoot Physiotherapy proudly operates on Jagera and Turrbul land. We acknowledge Traditional Owners of Country throughout Australia and recognise the continuing connection to lands, waters and communities.
We pay our respect to their Elders past and present and extend that respect to all Aboriginal and Torres Strait Islander peoples today.